Does tramadol act as an opioid?
by egpat Posted on 09-12-2017
Can you guess tramadol as an opioid? Can you believe that it is not so euphoric and addictive than other opioids?
Yes. You are right. Tramadol is a centrally acting opioid analgesic that can be used in various painful conditions without bothering much about potential addiction as with other opioids.
That’s great. Tramadol is an opioid with less addiction so is it stands as the best in this class?
You will agree with the answer as ‘no’ on reading to the end of this article.
How tramadol acts as opioid?
Fine, so first let’s start our discussion on its structure and how it can be named as opioid.
Let’s have one question.
Is it structure related to other opioids?
No, the structure of tramadol is neither related to natural opioids nor synthetic opioids.
Tramadol is a simply cyclohexanol derivative with N,N-(dimethylamino) methyl group at α-position.
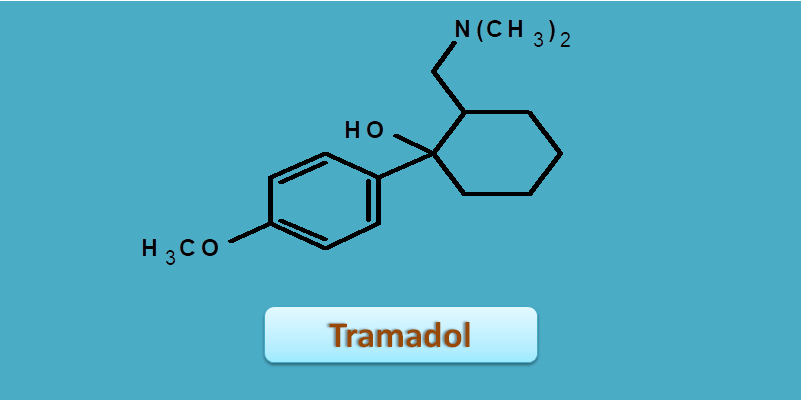
On the other hand, natural opioids like morphine, codeine and oxymorphone all have a common skeleton of five rings each varying at nature of substituent at various locations.
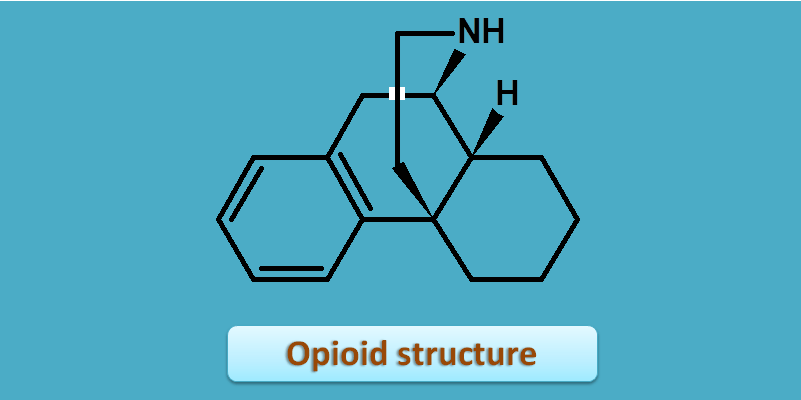
Alt: Structures of morphine, synthetic drugs
Even synthetic opioids like fentanyl and meperidine are somewhat related to natural opioids, of course with less number of rings but preserve some structural similarity.
Then, how can you call it is an opioid?
If you see the structure, it has no structural similarity with other opioids but still share their properties such as producing central analgesia.
Also it’s quite similar that tramadol produces constipation, nausea, dizziness just like opioids.
Can we call it is an opioid based on the above actions? Will all the drugs producing central analgesia are opioids?
Undoubtedly the answer is ‘No’. We can’t call it is an opioid by just considering its analgesic action but still we should have a bit more evidence.
Yes, one of the key factor, its mode of action.
Even it has no structural similarity and addiction potential as other opioids, interestingly it acts like opioids.
One of the proposed mechanisms for tramadol is its action on central μ-opioid receptors. Like other opioids, it binds to these receptors which cause hyperpolarisation of the neuronal membrane leading to suppression of pain signalling.
One of its metabolite shows more affinity towards μ-opioid receptors which may also take part in its role.
That’s great. So tramadol is an opioid with all favourable effects and minimal addiction and we have a best drug in our hand to control pain?
The smile on our face should have its limits by reading these facts.
No doubt, tramadol is less addictive than other opioids such as morphine and codeine but when used at recommended dose and for recommended use.
Even it looks like less euphoric, it can produce more euphoria and addiction when it is inappropriately used leading to drug abuse.
Another important concern is about its withdrawal effects.
Tramadol shows significant withdrawal effects such as anxiety, tremors, pain, insomnia, seating and nausea.
Again this is a strong indication of addictive nature of tramadol which precipitates symptoms just like other opioids on sudden stopping of its use.
Precipitation of seizures is another bottleneck to its use.
It’s very disappointing that tramadol can’t be used liberally and it should be checked for potential seizure risk generation when given with other drugs.
It can increase the risk of seizures in patients on treatment with other drugs like selective serotonin reuptake inhibitors (SSRIs) and tricyclic antidepressants (TCAs).
Now let’s see another face of tramadol.
It can precipitate few adverse effects like tachycardia, hyperthermia, agitation and hallucinations all the symptoms come under the roof called serotonin syndrome.
These side effects can be increase with concomitant use of other drugs like SSRIs, TCAs and MAO inhibitors.
Okay, let’s avoid this drug in these situations but why don’t we use it in other people who has no seizure or serotonin syndrome risk.
That’s not the end of tramadol story.
Suicidal initiation, a more significant risk, is coming into the play raising severe warning on tramadol’s liberal use.
The drug can increase suicidal initiation in patients with depression or drug abuse.
It’s alarming now.
Many of the chronic pain conditions may be associated with some sort of depression in the patients. So it’s very essential to check the status of the patient for any history depression or drug abuse.
That’s all about the drug of discussion here.
Conclusion
Now what we can conclude? Can’t we use tramadol? Is it risky?
Interestingly the above questions have two answers – ‘yes’ and ‘No’.
Yes, we shouldn’t use tramadol in patients with high risk of seizures, suicidal thoughts, drug abuse or under treatment with drugs like SSRIs, TCAs and MAOs to eliminate potential drug interactions.
No, use of tramadol is not a risk in all patients when it is properly checked for possible interactions and when it is used at a right dose for a right use.
Every drug will have its merits and demerits and it is just so with this case. Tramadol being an opioid shares similar risks as other centrally acting drugs but when used properly it can produce favourable effects.